Alabama Medicaid reforms first envisioned six years ago are finally going into effect today. And Alabama Arise will work hard to ensure Medicaid’s new structure keeps patient needs and consumer voices at the forefront.
The new plan brings regional control and care coordination of primary care services through seven Alabama Coordinated Health Networks (ACHNs) serving more than 700,000 Alabama Medicaid enrollees, mostly children. The ACHNs also will serve pregnant women and family planning patients. The networks, which officially launched today, will begin providing care coordination services Nov. 1.
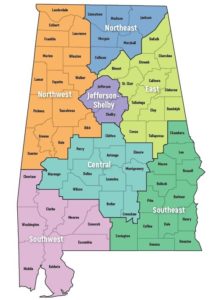
The goals: Healthier patients and a strong consumer voice
For the first time, Alabama Medicaid governance will include consumer voices at the policy table. Each ACHN will have a Consumer Advisory Committee as well. Arise and our advocacy partners are pleased with this accountability provision and are working to strengthen consumer oversight.
Arise has partnered with the Alabama Disabilities Advocacy Program and the Disabilities Leadership Coalition of Alabama to recruit consumer representatives for the new roles. Together, we held a training for the group on Sept. 20. A major goal of Arise’s Medicaid consumer advocacy is to help the regional representatives work together as a statewide team.

In addition to the new consumer voices, we’re hopeful about the plan’s emphasis on improving health outcomes. Each ACHN will receive funding to develop and implement Quality Improvement Projects (QIPs) targeting three initial quality measures: (1) childhood obesity, (2) infant mortality and birth outcomes and (3) substance use disorders. Doctors will be eligible for bonus payments for meeting or exceeding goals on numerous care coordination and quality measures.
Arise will seek to ensure the QIPs reflect and respond to community needs. We’re working particularly closely with local partners in Mobile to bring community input into the QIP design process there. Stay tuned for more information about our food security work in the Trinity Gardens neighborhood!
Compare and contrast with past reforms
The Legislature voted overwhelmingly in 2013 to create Medicaid regional care organizations (RCOs) to cut costs and promote preventive care. But Gov. Kay Ivey, citing delays and budget problems, used an escape clause in the law to abandon RCOs in 2017.
The new ACHNs resemble the former RCOs, with a few key differences. Under the RCO plan, Medicaid would have given private, nonprofit managed care organizations a set monthly payment for each Medicaid enrollee (or member) in their region. The organizations, in turn, would have assumed full financial risk if overall costs exceeded those payments.
ACHNs also involve private nonprofit contractors, but payments will be based on medical services and care coordination services provided. The organizations also will assume only partial financial risk.
How the new ACHNs will work
The ACHNs will coordinate primary care for people with Medicaid coverage. Your ACHN will have a phone line to call when a Medicaid member has a health problem.
New services will help patients get the health care that’s right for their needs. To get these services, people who have Medicaid coverage (children, pregnant women, and people getting family planning services) will need to have a primary care doctor of their choice.
Their doctor will become their “medical home” – the first place to contact for ordinary health needs. And new services will be offered to improve patient health.
Medicaid members who already have a primary doctor can continue under their care. Coordinating patient care through a primary doctor helps avoid expensive emergency room visits for routine health care needs.
Other Medicaid reform efforts underway
ACHNs are the next step down the reform path for Alabama Medicaid. In October 2018, the agency launched a new statewide Integrated Care Network (ICN) to serve Medicaid long-term care patients. About 16,000 of the ICN members live in nursing care facilities. Another 9,000 receive long-term care services at home or in their communities through Medicaid waivers.
The state’s 13 regional Area Agencies on Aging provide the care coordination services for the statewide ICN. And as with ACHNs, Arise is working to ensure a strong consumer voice in the ICN. Arise has a seat on the ICN Consumer Advisory Committee, as well as an appointee on the ICN board.
Alabama’s Medicaid reforms are an encouraging move toward more patient-centered care. The inclusion of consumer voices and the emphasis on care coordination for quality improvement have the potential to move the needle on some of Alabama’s most persistent health challenges.
That would be a win for hundreds of thousands of Alabama Medicaid members – and for the whole state.

